Dance Stance
This variation of your massage stance can reduce discomfort, help conserve strength, and use your movement and body weight most efficiently during a session.
Clients with nonspecific low-back pain may be experiencing mechanical wear and tear of the zygapophyseal joints, located in the posterior aspect of the lumbar spine (Image 1). These bony articulations are commonly referred to as facet joints, but the proper terminology is zygapophyseal joints or Z-joints—derived from the Greek words zygos, meaning bridge, and physis, meaning outgrowth. The Z-joints are lined with cartilage, lubricated in synovial fluid, and covered by a tough joint capsule. When healthy, they allow smooth gliding and sliding while preventing excessive lumbar rotation.
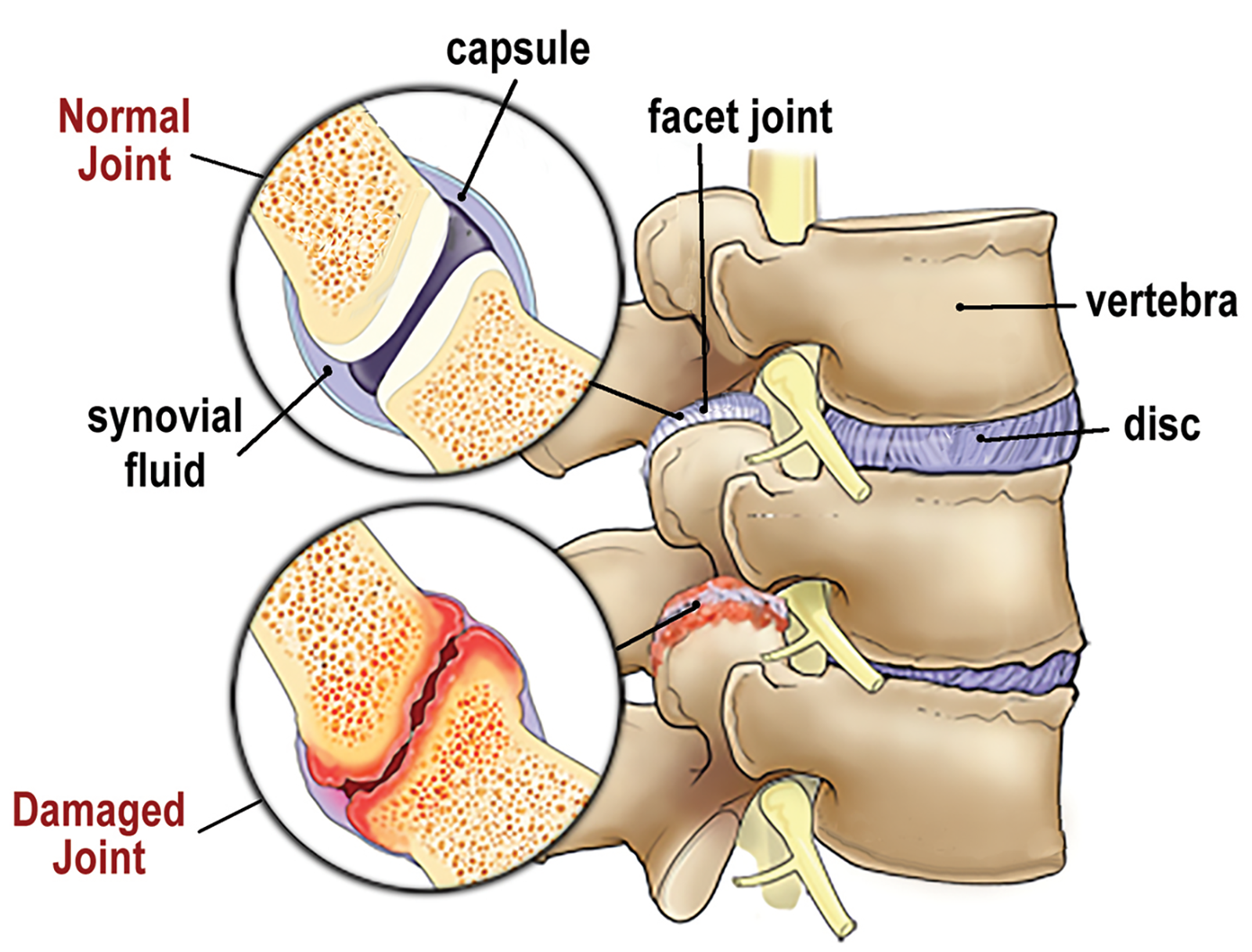
In the middle-aged and elderly populations, normal vertebral motion is often compromised, or an injury, repetitive movements, obesity, weak posture, and aging articular cartilage may change the way the Z-joints align and move on one another. Additionally, trauma combined with prolonged gravitational exposure causes thinning of the joint capsule, cartilage degradation, and accompanying bone spurs.
Similar to knee arthritis, the changes in the physiology of the Z-joints make it difficult for the joint to move fluidly, which often triggers an inflammatory response. With chemically sensitized medial branch sensory nerves bombarding the spinal cord and brain with danger signals, the back stiffens and may hurt during certain movements.
Acute episodes of lumbar Z-joint pain are typically intermittent, generally unpredictable, and occur a few times per month or per year. Although standing may be somewhat limited, sitting seems to be the most provocative position. In acute cases, Z-joint symptoms typically localize to one side of the back adjacent to the spine. In chronic cases, diffuse pain may spread into the buttock, groin, or down the entire limb.
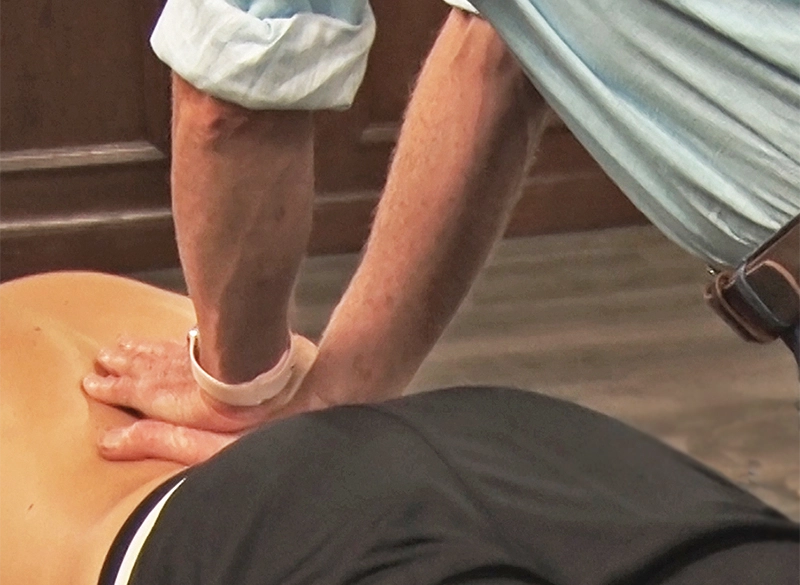
In Image 2, I begin assessment by gently palpating the paravertebral tissues overlying the lumbar transverse processes. The Z-joints themselves are not manually palpable, but this maneuver is helpful in localizing and reproducing any point tenderness, which commonly accompanies Z-joint mediated pain. If the client reports localized unilateral tenderness, there are several confirmation exams I've found helpful, especially the Sphinx Hyperextension Test (Image 3).
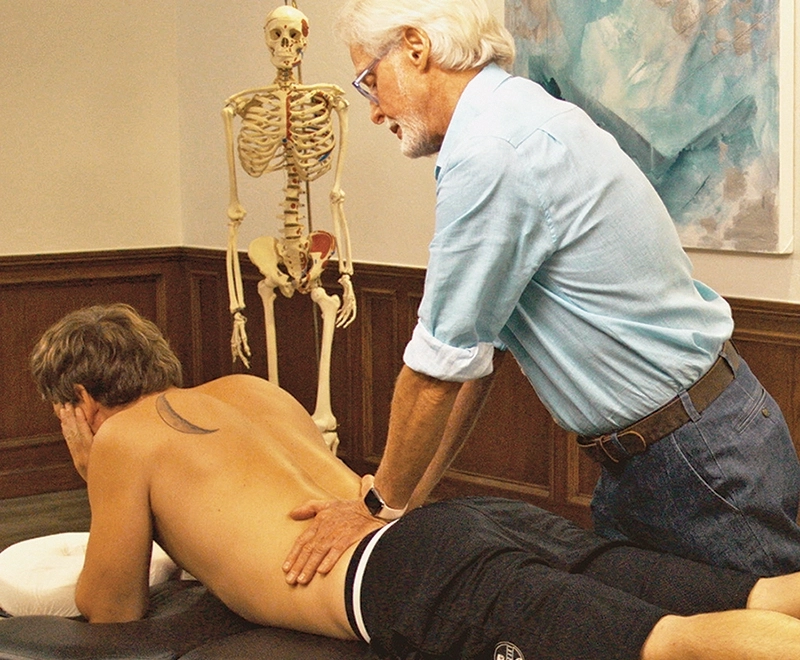

In the Kemp's Test (Image 4), backward bending, rotation, and sidebending toward the affected side may elicit Z-joint symptoms. However, it's important to note that this pain provocation test may also implicate nerve root compression and sciatica symptoms. Sharp buttock and leg pain following a dermatomal pattern may suggest sciatica, whereas Z-joint irritation is suspected if the test reproduces the client's localized low-back pain. If unsure, several other tests, such as the Slump Test and Straight Leg Raise Test, should be clustered to confirm your findings.
Numerous studies have examined conservative care for people with low-back pain, but I'm unaware of any published investigations that have targeted Z-joint pain specifically. Nevertheless, most experts agree that the general principles of conservative treatment for nonspecific low-back pain can be applied to Z-joint pain too.1
I've had reasonable success treating both acute and chronic cases of Z-joint pain using the Myoskeletal Alignment Techniques (MAT) demonstrated in Images 5 and 6. These graded-exposure stretching maneuvers are designed to bring balance to musculofascial tissues that torsion the pelvic bowl and create excessive anterior pelvic tilt. When performing these dynamic postural stretching routines, it is best to address all connective tissues that articulate with the lumbar spine, hips, and legs that may be creating abnormal compressive loading through arthritic Z-joints.

Image 5. Passive Sidebending Technique: With his right hand bracing the client's thigh, the therapist's left hand sidebends the client's lumbar spine to stretch the quadratus lumborum and decompress the Z-joints on the client's right side. The client is asked to gently right sidebend against the therapist's resistance to a count of five and relax, and the therapist again left sidebends the client to the next restrictive barrier. Repeat 3-5 times and retest using the Kemp's Test.
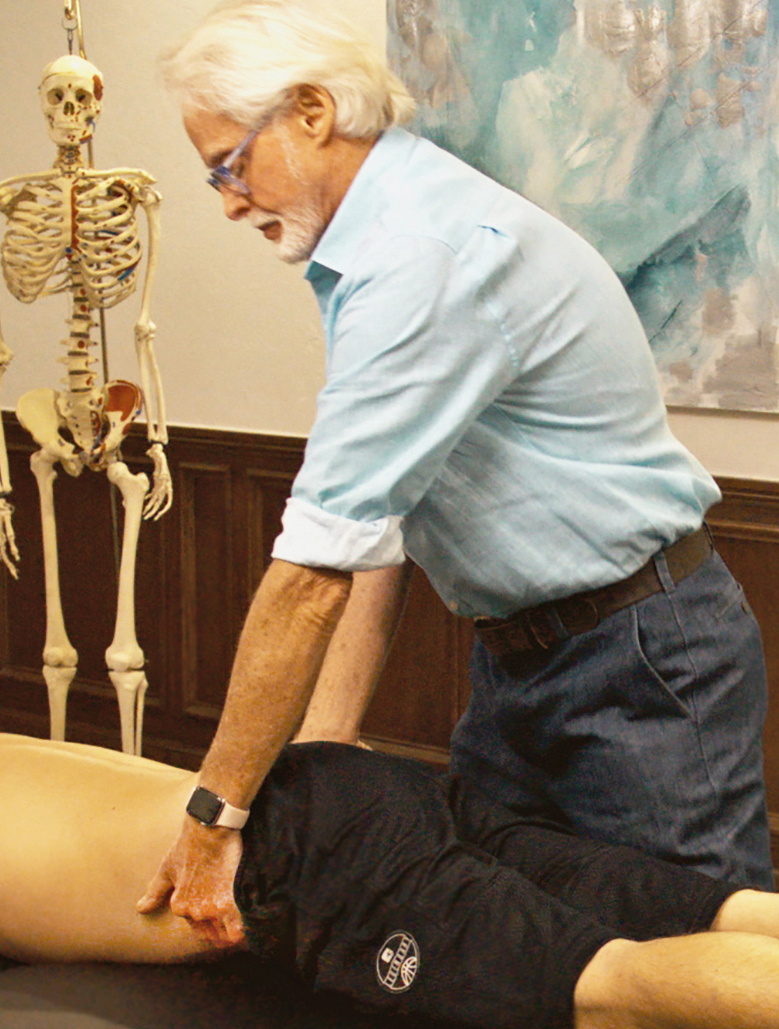
In short, MAT treatment goals for Z-joint pain include:
During each therapy session, feel free to offer advice about various sitting and standing postures that may help relieve compressive stress through the Z-joints. Cueing the client about faulty movement patterns helps bring the brain's attention to protectively guarded areas. All movements are governed by the central nervous system, so the brain will limit flexibility, range of motion, and mobility if it feels there is a potential danger. Therefore, it's important to always maintain good communication with clients and keep them actively engaged in the therapy process. While Z-joint arthritis can't be dramatically reversed, I've found that exercise, lifestyle changes, and proper bodywork can contribute to a better quality of life and less discomfort.
1. David S. Binder and Devi E. Nampiaparampil, "The Provocative Lumbar Facet Joint," Current Reviews in Musculoskeletal Medicine 2, no. 1 (March 2009): 15-24, https://doi.org/10.1007/s12178-008-9039-y.
This variation of your massage stance can reduce discomfort, help conserve strength, and use your movement and body weight most efficiently during a session.
Caring for elderly clients requires the massage therapist to have a keen awareness, not only of the characteristics unique to the client but also of the various members of the client’s care team.
Changing muscle memory habits as they relate to mobility and movement can be hard. Luckily, you are there to help clients along so they aren’t forging a new path alone.
While tension-reducing techniques can help when issues arise from forward-head posture, addressing joint restrictions through manual therapy can prove more significant.